Questions remain about the respiratory risk posed to a fifth of the United States population by increasing wildfires—but a CU Boulder researcher is trying to clear the air
It had already been an exceptional fire season across the American West by the time Montana’s Rice Ridge fire ignited.
It began in July 2017 as many western wildfires do: with a dry lightning strike on a parched patch of plant litter. Immediately it stirred an inferno that stretched for miles and, by September, consumed an area of forest almost twice the size of Denver, producing enough thick smoke to choke half of the country.
“It’s been described to me in apocalyptic terms,” Sarah Coefield, an air quality specialist with the Missoula City-County Health Department, told the Washington Post at the time about the area surrounding the fire.
The orange plumes of ash were so dense that Coefield commented in that same interview that, “Visibility has been down to less than a block.”
Miles away from Montana, that same thick, orange haze, accompanied by the ash of other wildfires in California, Oregon and Washington, heaved its way across the rolling hills of the Midwestern tallgrass prairies—and they weren’t alone in their suffocation.
Before all was said and done, this smoke—accumulated from dozens of wildfires—had hijacked the meandering jet stream, getting a first-class ticket to blanket more than 3,000 miles of middle America. It ultimately traveled as far east as New York and Pennsylvania and as far south as Texas, and illustrated yet another example of a new normal for those in and out of the Smoke Belt.
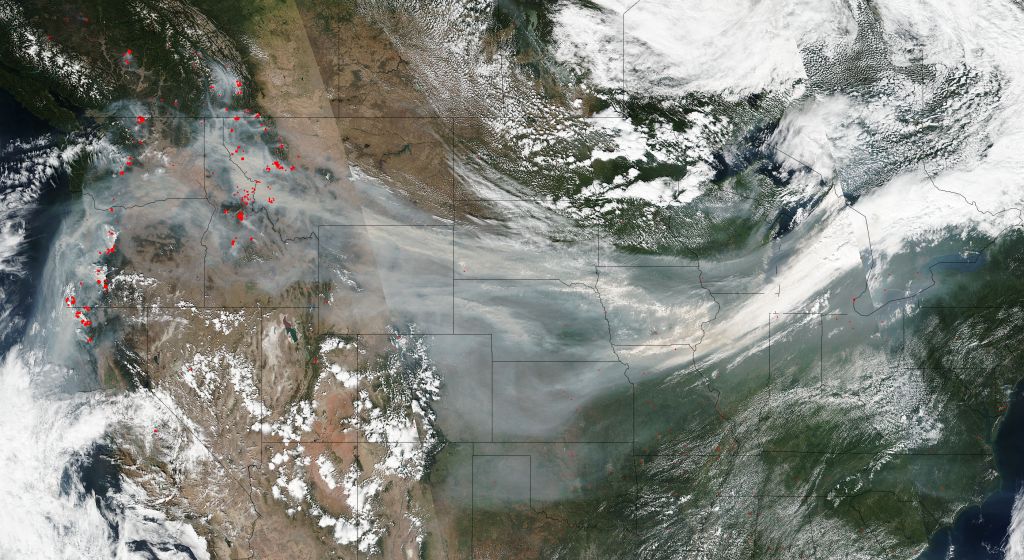
Wildfire smoke—like wildfire itself—is becoming more common and more powerful due to a changing climate, affecting communities from California to the Pacific Northwest, and from the Pacific Ocean east to the Great Plains. And yet, the documented public health effects of smoke remain relatively unknown, and, for what does exist in the research, inconsistent with a few important exceptions.
But a researcher at the University of Colorado Boulder seeks to change that, particularly for those distant fires that share their smoke.
“When we think about all of the things in the future that might be changing that influence wildfire risk and health impacts, there’s so many things,” said Colleen Reid, an assistant professor of geography at CU Boulder who studies the impact of wildfire smoke on public health. “You can’t keep fire at bay.”
The difficulty in discerning the health effects of smoke stems from the very nature of the plumes, and the U.S. approach to tracking it. Currently, there are air pollution monitors set up by the Environmental Protection Agency across the United States—often near metropolitan areas—with the goal of assessing whether air pollution regulations are working. These monitors, however, don’t always measure every day, meaning that if the wildfire is moving fast or the smoke is only hovering temporarily, they could miss the data from the high levels of smoke altogether.
Reid, though, approached this problem from three perspectives in order to improve understanding of the potential health impacts: She conducted a critical review of all existing literature on the public health impacts of wildfire smoke exposure, she researched the birth weight of babies whose mothers were exposed to smoke while pregnant, and then she specifically examined the 2008 California wildfires and their corresponding respiratory health effects for downwind populations.
At the time, the 2008 California wildfires were one of the largest fire events in the state’s history. Ignited by more than 6,000 lightning strikes, this fire event consisted of thousands of blazes raging across 26 counties in the northern half of the state.
As structures and trees burned, fine particulate matter—or the incredibly small, easily inhalable solid and liquid particles suspended in the air during a high pollution event—coated the state.
These particles—or what makes the “haze” of wildfires—aren’t just the remains of burned trees. They can also be the debris particles of human products like plastics, electrical wires and spray foam insulation, or anything else that may have gotten in the fire’s path. And, while just one of the many hazards that accompany wildfires and air pollution more broadly, it is in many respects the most dangerous for human health.
Particulate Matter is often measured in two forms: Particulate Matter 2.5 (PM2.5) and Particulate Matter 10 (PM10). PM2.5 are the fine inhalable particles that measure particles that are roughly 2.5 micrometers or smaller, while PM10 are roughly 10 micrometers and smaller. These particles—which are roughly the length of an E. coli bacterium and a single fog, mist or cloud water droplet, respectively—are so small that they can easily penetrate the lung’s alveolar sacs, which are partly responsible for exchanging oxygen between the lungs and the blood stream, and corrode its walls.
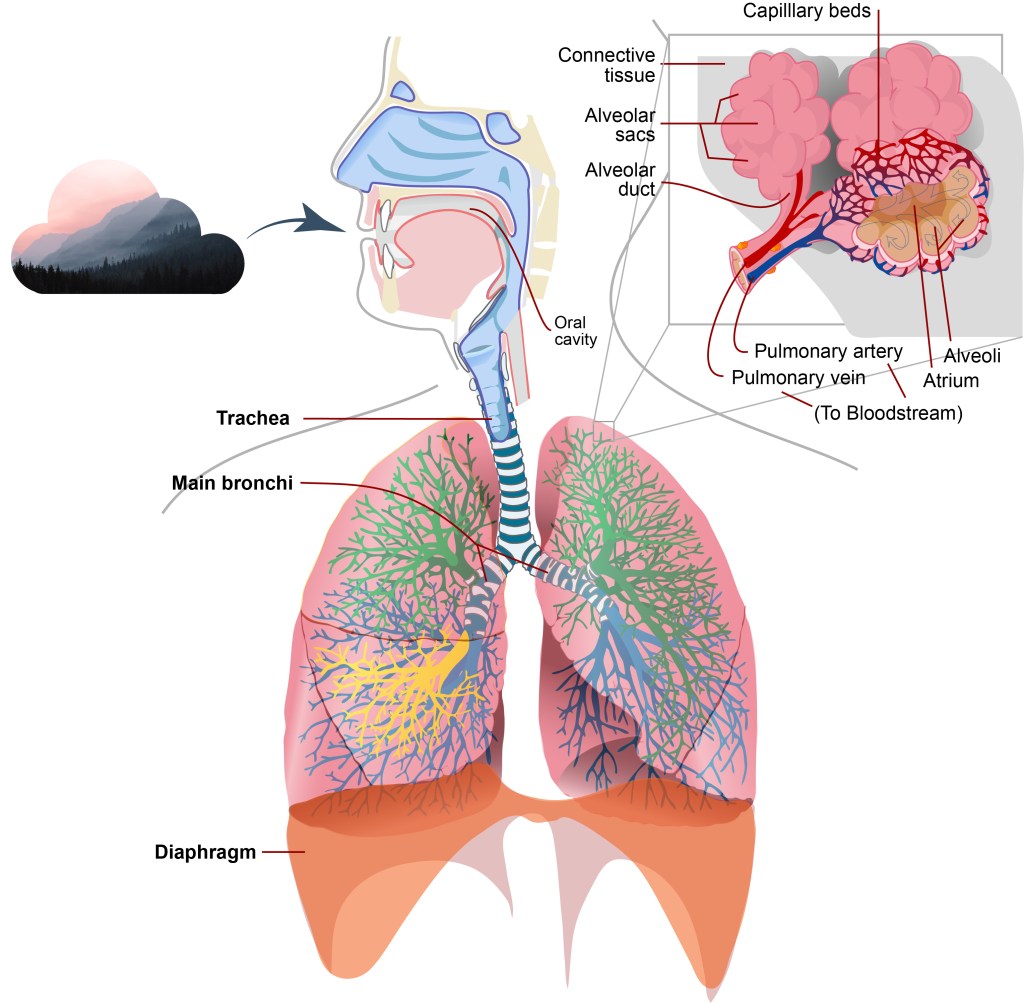
In other words, they are able to bypass all of the body’s defenses, going straight into the blood.
Given this effect on the body, the World Health Organization has recommended that there be no minimum threshold where humans are safe to breathe in particulate matter from human-caused air pollution, which has been linked to 25 percent of lung cancer deaths, 8 percent of chronic obstructive pulmonary disease (COPD) deaths and 15 percent of heart disease and stroke cases.
And the effects don’t stop there. While sensitive populations—the young, the old, the sick—are much more vulnerable, even perfectly healthy people can feel the impact of high particulate matter through irritation to the lungs, eyes and skin, an increased risk of respiratory tract diseases and cardiovascular diseases, reduced lung function, the development of an irregular heartbeat, nonfatal heart attacks, and even premature death.
With wildfire smoke, there is a widespread consensus among researchers that these plumes do exacerbate respiratory diseases such as asthma and COPD and can cause an increased risk of death for sensitive populations, but in terms of the other effects, there is still a lack of agreement—particularly for those impacted downwind.
Right now, the EPA has the daily limit of all pollution related to fine particulate matter (PM2.5) set at 35 µg/m3 (micrograms per meters cubed). Ideally, with good clean air, the levels would be below 12 µg/m3. But, even at 35 µg/m3, most people (with the exception of sensitive populations) may not notice any sort of change or difficulty to their breathing.
“The fire that I studied, it (the particulate matter) maxed out close to 300 µg/m3. The Napa fires that were just happening… there were values in the 400s. So, it’s really, really bad,” said Reid. “Even San Francisco and Oakland were getting levels that were in the high 100s, low 200s, and that’s an area that tends to have pretty good air quality. So, it’s much higher than they’re used to.”
For Montana, much like California, this was the summer of smoke, with Seeley Lake—near where the Rice Ridge fire took place—experiencing record levels of smoke at 18 times what the EPA deems safe, and even breaking the air monitoring device for five hours because the pollution was simply higher than the device’s limit.
Despite this, the Front Range, and Colorado more broadly, was relatively clear and quiet. For most of the summer, the PM2.5 levels stayed within the healthy limit (normally between 0 and 20 µg/m3), well below the EPA’s limit. When Montana’s smoke begun its thick descent into the Denver metro, though, the levels spiked to between 40 and 50 µg/m3. Boulder’s jump was even more impressive, getting above 50 µg/m3 for the week of exposure.
During that time, health officials at National Jewish Health in Denver told the Denver Post that they had seen an uptick in patients reporting a shortness of breath and coughing episodes, as well as Prednisone prescriptions—all of which are common during high air pollution events, called “Action Days,” along the Front Range.
The possible health effects from those exposed during these Action Days—which are issued by the Colorado Department of Public Health & Environment for any number of air pollution issues, including any days with high particulate matter—are complicated, just like any issue related to public health.
“Severity is more related to the severity of the underlying disease than to the intensity of the exposure,” said Karin Pacheco, an allergist at National Jewish Health and an assistant professor in environmental and occupational health at the University of Colorado Denver.
We’re always going to have wildfires in the West. … So, we need to figure out how to protect health.
Colleen Reid, assistant professor of geography, CU Boulder
Similar to how healthy individuals can have differing reactions to differing levels, those among the sensitive populations—and particularly children who breathe much faster and are much more susceptible—can also have different reactions despite the original source of the pollution.
“It all is equally as horrible for the lungs,” said Lauren Massie, an undergraduate student at CU Boulder in English who suffered from severe, childhood asthma, and still suffers complications if the air pollution is too bad. “I still need to take precautions.”
Those recommended precautions to avoid the pollution, outlined by the CDC, tend to revolve around avoiding particulate matter in particular. They suggest, first and foremost, to check local air quality reports and visibility guides (which can be an indicator as to the level of particulates in the air). And, if there is anything, to stay indoors.
“Unfortunately, keeping safe on high smoke days means avoiding exposure,” commented Pacheco.
Even inside, there are a number of steps that can be taken to keep the air clear, including keeping the fresh-air intake closed, avoiding any activities that might increase indoor pollution (such as using your fireplace or burning any candles) and keeping your HVAC air filter clean.
While thus far there have been no long-term health impacts linked to smoke exposure (like what has been seen with other high-particulate matter events), the reality is that there just isn’t enough information or research yet. And, with the length of the wildfire season projected to triple, and hit closer than ever to major urban corridors due to human interference, a public health crisis of toxic air may be looming for the western United States.
Researchers, including Reid, are working on documenting these health effects for those downwind by improving the literature and watching different fire events closely, but the work is slow, expensive and extensive—and, she said, important.
“We’re always going to have wildfires in the West,” acknowledged Reid. “So, we need to figure out how to protect health.”
Republished with permission from the Colorado Arts and Sciences Magazine, where it was published in 2018.
